Home
This model is an individual (or micro-simulation) model designed to support decision-making regarding population screening for colorectal cancer (CRC) at the state level. The model is comprised of the following parts:
- Demographics
- Natural history
- Testing and treatment for CRC
Based on assumptions regarding trends in demography, natural history, screening dissemination and accuracy, and intervention reach and efficacy, the model simulates cancer incidence and mortality by stage, age, and calendar year.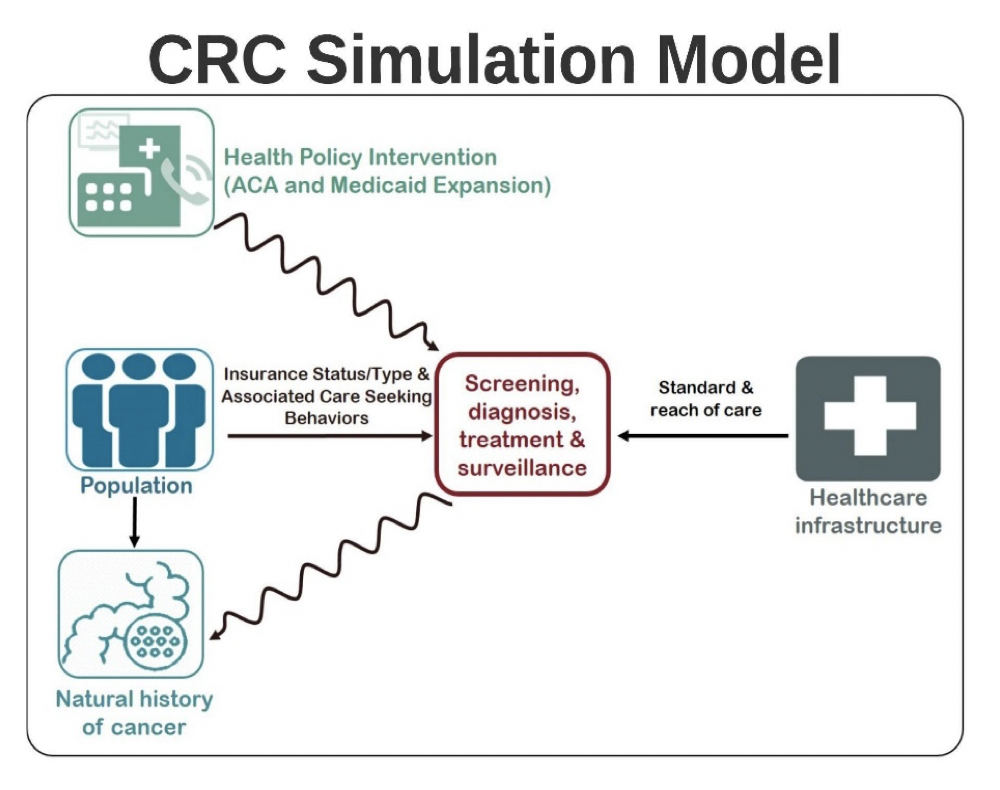 As shown in the above figure, CRC screening, diagnosis, treatment, and surveillance are influenced by healthcare infrastructure, including healthcare quality and access, health policy interventions, such as those that affect access to insurance, and health behaviors. These CRC screening and surveillance rates can then change an individual’s natural history of cancer, such as through the removal of polyps and cancerous lesions. Our model seeks to measure the impact of health policy interventions on CRC screening and outcomes.
As shown in the above figure, CRC screening, diagnosis, treatment, and surveillance are influenced by healthcare infrastructure, including healthcare quality and access, health policy interventions, such as those that affect access to insurance, and health behaviors. These CRC screening and surveillance rates can then change an individual’s natural history of cancer, such as through the removal of polyps and cancerous lesions. Our model seeks to measure the impact of health policy interventions on CRC screening and outcomes.
Capabilities
The model is an individual-level simulation environment that includes input data on the population, screening patterns, cancer progression, cancer outcomes, costs, and the effects of interventions and policies. The model is geo-spatially explicit and can be extended for use in specific geographic regions and sub-populations as well as for other types of cancer. Specifically, it has the functionality to perform the following:
- Integrate multiple data sources to evaluate the effects of specific policies and interventions
- Simulate the behaviors, experiences, and outcomes of realistic and diverse populations]
- Account for local nuances and differential impact of interventions in different contexts
- Quantify the expected uptake and health and economic impact of specific interventions and policies in specific contexts, settings and sub-populations
- Forecast outcomes over long time periods, with attention to uncertainty
- Model combinations of interventions to understand potential interacting, synergistic, or ceiling effects when attempting to encourage specific health behaviors within a population
- Assess the full continuum of cancer care outcomes, such as: cost per person screened, cost per cancer case averted, and cost per life-year gained
Use in Decision-Making:
This approach provides opportunities to inform policies, interventions, and strategies related to CRC prevention, screening, and treatment among a variety of stakeholders. Additionally, this approach supports selection and implementation of interventions best suited for local contexts and sub-populations.